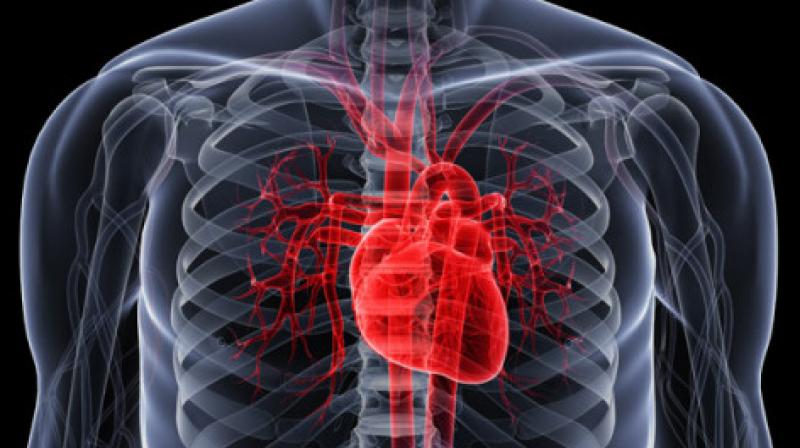
Cardiomyopathy is a group of diseases that affect the heart muscle, impairing its ability to pump blood effectively. This can lead to heart failure, arrhythmias, and other complications. Cardiomyopathy can be caused by various factors, including genetics, underlying medical conditions, and lifestyle choices. There are several types of cardiomyopathy, with the most common being:
- Dilated Cardiomyopathy (DCM): The heart’s main pumping chamber (left ventricle) becomes enlarged and weakened, reducing its ability to pump blood efficiently.
- Hypertrophic Cardiomyopathy (HCM): The heart muscle thickens abnormally, making it harder for the heart to pump blood and increasing the risk of arrhythmias.
- Restrictive Cardiomyopathy: The heart muscle becomes stiff, preventing it from filling properly between beats. This limits the heart’s ability to pump blood effectively.
- Arrhythmogenic Right Ventricular Cardiomyopathy (ARVC): A rare form in which the muscle tissue in the right ventricle is replaced by scar tissue, leading to arrhythmias.
Symptoms and Causes
Symptoms: The symptoms of cardiomyopathy can vary depending on the type and severity of the disease. In the early stages, some people may not experience any symptoms, but as the disease progresses, symptoms may include:
- Shortness of breath, especially during physical activity or while lying flat
- Fatigue and weakness
- Swelling in the legs, ankles, and feet (edema)
- Chest pain or discomfort
- Irregular heartbeats (arrhythmias), palpitations, or fluttering sensations in the chest
- Dizziness, lightheadedness, or fainting
- Persistent coughing, especially at night
In severe cases, cardiomyopathy can lead to heart failure or sudden cardiac arrest.
Causes: Cardiomyopathy can have a range of causes, including:
- Genetic Factors: Many cases of hypertrophic and dilated cardiomyopathy are inherited, with a family history of the disease increasing the likelihood of developing it.
- High Blood Pressure: Chronic high blood pressure can cause the heart muscle to thicken or weaken over time.
- Coronary Artery Disease (CAD): Blockages in the coronary arteries can damage the heart muscle and contribute to dilated cardiomyopathy.
- Infections: Viral infections, particularly myocarditis (inflammation of the heart muscle), can lead to cardiomyopathy.
- Alcoholism or Substance Abuse: Chronic alcohol or drug use can damage the heart muscle and lead to dilated cardiomyopathy.
- Nutritional Deficiencies: Lack of essential nutrients, such as vitamins and minerals, can affect heart health.
- Chemotherapy or Radiation: Treatments for cancer, such as certain chemotherapy drugs or radiation therapy, can damage the heart muscle.
- Autoimmune Diseases: Conditions like lupus or rheumatoid arthritis can lead to cardiomyopathy.
Diagnosis and Treatment
Diagnosis: Diagnosing cardiomyopathy typically involves a thorough physical examination, a review of medical history, and various diagnostic tests, including:
- Electrocardiogram (ECG/EKG): This test records the heart’s electrical activity to detect abnormal heart rhythms or other electrical problems.
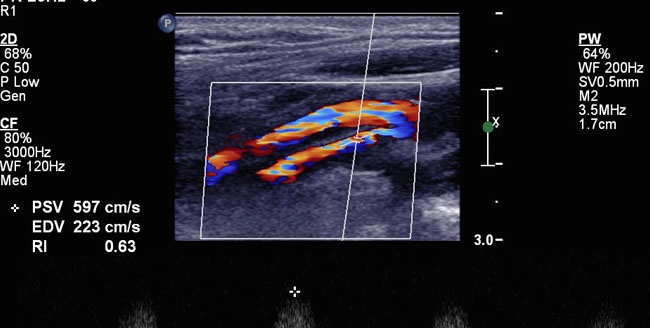
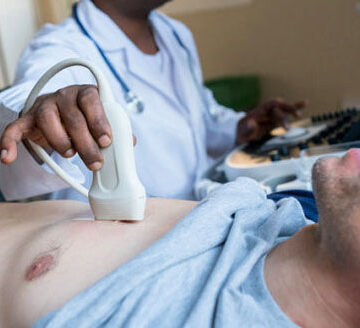
- Echocardiogram: An ultrasound of the heart that provides detailed images of the heart’s structure and function, helping assess the size, thickness, and motion of the heart muscle.
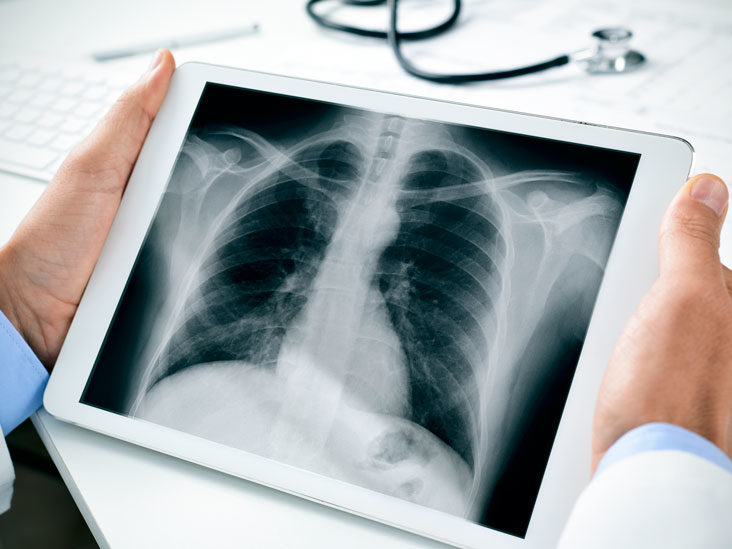
- Chest X-ray: This can show whether the heart is enlarged or if there is fluid buildup in the lungs, indicating heart failure.
- Cardiac MRI: Provides detailed images of the heart to assess heart muscle damage or scarring.
- Blood Tests: To check for markers of heart failure, infection, or other conditions contributing to cardiomyopathy.
- Stress Test: A test to monitor how the heart performs under physical stress, which can reveal issues with the heart’s pumping ability.
- Cardiac Catheterization: A procedure where a catheter is inserted into the heart to evaluate blood flow, pressure, and the function of the heart chambers.
Treatment: The treatment for cardiomyopathy depends on the type and severity of the condition but generally focuses on managing symptoms, preventing complications, and improving heart function. Common treatments include:
- Medications:
- Beta-Blockers or ACE Inhibitors: To reduce the heart’s workload and help it pump more efficiently.
- Diuretics: To reduce fluid buildup in the body, easing symptoms of heart failure.
- Anticoagulants: To prevent blood clots, especially in patients at risk of stroke or other complications.
- Antiarrhythmic Medications: To control irregular heartbeats and prevent dangerous arrhythmias.
- Lifestyle Changes:
- Maintaining a heart-healthy diet low in sodium, fats, and sugars.
- Regular physical activity under the guidance of a healthcare provider.
- Quitting smoking and reducing alcohol intake.
- Managing risk factors such as high blood pressure, diabetes, and high cholesterol.
- Implantable Devices:
- Pacemaker: A small device implanted under the skin that helps regulate slow heartbeats.
- Implantable Cardioverter-Defibrillator (ICD): A device that monitors heart rhythms and delivers shocks if dangerous arrhythmias are detected, preventing sudden cardiac arrest.
- Left Ventricular Assist Device (LVAD): A mechanical pump implanted in patients with severe heart failure to help the heart pump blood more effectively.
- Surgery:
- Septal Myectomy: A surgical procedure to remove part of the thickened heart muscle in hypertrophic cardiomyopathy, improving blood flow.
- Heart Transplant: In severe cases of cardiomyopathy, where other treatments fail, a heart transplant may be considered as a last resort.
When to See a Physician
You should see a doctor if you experience any of the following:
- Persistent shortness of breath, especially during routine activities or while lying down
- Frequent episodes of chest pain or discomfort
- Irregular heartbeats or palpitations
- Swelling in your legs, ankles, or feet
- Unexplained fatigue, dizziness, or fainting
Additionally, if you have a family history of cardiomyopathy or heart failure, you should consult a doctor for regular check-ups and screenings, as early detection can help manage the condition and prevent complications.
Benefits of Early Diagnosis and Treatment
- Prevention of Heart Failure: Early diagnosis and treatment can prevent cardiomyopathy from progressing to heart failure, which can lead to a better quality of life.
- Symptom Management: Proper treatment can significantly reduce symptoms like shortness of breath, fatigue, and swelling, allowing patients to return to their daily activities with less discomfort.
- Reduced Risk of Complications: Treating cardiomyopathy can help prevent life-threatening complications such as stroke, arrhythmias, and sudden cardiac arrest.
- Improved Prognosis: With early intervention, medications, lifestyle changes, and devices, many patients with cardiomyopathy can live long, healthy lives.
In conclusion, cardiomyopathy is a serious heart condition that can affect individuals in various ways. However, with early diagnosis, personalized treatment plans, and lifestyle modifications, patients can effectively manage symptoms, prevent complications, and improve their overall heart health and quality of life.